Medial Tibial Traction Periostitis
"I’ve got shin splints doc”! Of all the terms that stick with injuries, this is one of the die hards. The term ‘Shin splints’ is very broad and does not aptly describe the underlying process. A more appropriate term is medial tibial traction periostitis (Brukner & Khan 2007).
For ease of discussion it will be referred to as medial tibial pain.
Medial tibial pain is a common presentation to health professionals on a daily basis and usually arrives as a chronic case. The typical distance running scenario is ongoing for 6 months or more with many homecare interventions such as rest, stretching of the calves, anti-inflammatory medication, heat application, new shoes and the cycle continues.
Anatomy
The lower limb interacts and is largely affected by the pelvis above (biomechanics are huge in this) and affects the positioning of the foot. The 3 major tissues that play a role in medial tibial pain in the lower limb are the soleus (lower calf) attaching onto the posterior portion of the tibia and fibula, the flexor digitorum longus (these flex the toes) also attaching to the posterior tibia and the tibialis posterior attaching to the posterior tibia and fibula and attaching the navicular (above medial arch) and base of metatarsal (base of toes)
These muscles attach to the bone via an attachment onto the periosteum. The periosteum is susceptible to large friction and traction forces in the lower one third of the tibia.
Onset
The more chronic case may be more resistant with a higher re occurrence rate. A chronic case may be 3-6 months with some cases lasting for up to 2 years
Treat this early - your options are;
ext-align: justify; text-justify: inter-ideograph;">
With the continuation of training, pain will gradually increase to the whole training session. Ultimately it can stop training altogether.
Causes
The usual loading factors play a large role in the onset of medial tibial pain such as;
- Increase in volume
- Increase in intensity
- Fatigue (usually involved with the above factors)
- Increase in hard surface running
- Excessive pronation
- Biomechanics – stride length, pelvic position, pelvic stability
- Decreased recovery time between training bouts
What is very important to understand is the periosteum covers the bone as an attachment point for muscles and other connective tissues. Continual loading and tension on this site can lead to bone strain – a pre cursor to bone stress reactions. Early intervention is the key.
Treatment
From a clinical perspective the most important aspect is knowing the causative factor(s), though in the chronic case it is likely to be multifactorial.
Knowing the anatomy and the traction forces being placed on the periosteum of the bone we can start to understand what might be occurring. Tibial bending and torsion are large in the distal tibia during locomotion. During the gait cycle uncontrolled pronation during mid stance places an eccentric ‘pulling’ on the periosteal junction. This continual ‘pulling’ causes an inflammatory response evoking painful stimuli.
Addressing the eccentric forces and the control (rate) of pronation is often helpful. This can be achieved by strengthening of the tibialis posterior and flexor digitorum longus, thus decreasing the traction forces on the tibia.
Pronation control is also aided by adequate pelvic stability during the gait cycle. Further, pronation is affected by overstriding which in turn may be reliant on pelvic angle. It is always prudent to address biomechanics when medial tibial pain is experienced.
Soft tissue therapy may be helpful in areas of focal thickening and increased tone. Joint and soft tissue health can also be assessed as a possible factor.
Prognosis
In a fresh case (less than a few weeks) and the appropriate management usually there is a good response in approx. 2-4 weeks
The more chronic case may be more resistant with a higher re occurrence rate. A chronic case may be 3-6 months with some cases lasting for up to 2 years
For the best prognosis catch it early!!
Is further investigation warranted?
If you have been on the treatment merry-go-round and your pain is not improving (or worsening) then it might be wise to visit a sports physician who may be able to order some imaging studies. A range of imaging studies may be helpful.
Bone scan can be handy in detecting possible stress reactions however, according to Dr Tom Cross (Sydney based sports physician) one bone scan is equivalent to a radiation dose of 69 chest X-rays. That’s a big dose in one sitting! MRI’s may be effective in detecting local oedema and any soft tissue changes.
Even with further investigation, return to running is based on clinical features rather than return to normal appearance on imaging (imaging features may take months to years to return to normal despite absence of signs and symptoms) - it’s also expensive!
In summary
Treat this early - your options are;
- Ice
- Short term anti-inflams may be helpful
- Load/program modification (rest may be helpful initially)
- Biomechanics
- Taping and foam application (de-loading tibial area)
- Soft tissue therapy
- Tibialis posterior strengthening
- Pronation control
- Stretching exercise, if it is identified there are restricted soft tissues
- Joint mobilisation
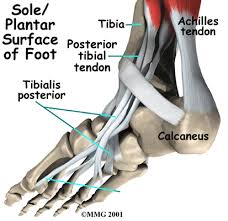
Figure 1 - The tibialis posterior becomes superficial in the medial (inside) ankle. You can see how weakness in this will predispose to pronation causing a 'traction' effect on the medial tibial border. This often irritates the periosteum.
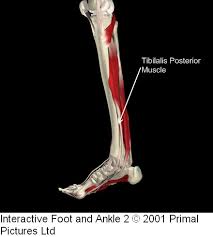
Figure 2 - The tibialis posterior tendon can be seen in the lower one third of the tibia on it's course to the attachment under the foot.
Strengthening
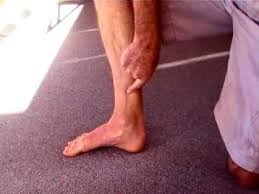
Figure 3 - Ideally strengthening would be performed in a standing position. Keeping the heel and the ball of foot on the ground lift the arch up 1-2cm (this will be hard to activate at first), then slowly lower. To increase difficulty hold this position and lift the heel 2-3cm off the ground, then slowly lower.
If you have a rigid foot in a static position you will probably have less available movement. These are stabilsing muscles therefore they will probably do better with multiple stes and reps throughout the day ie; 4 sets 4-6 reps (building to 10+) 3-4 times per day.
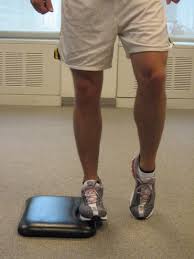
Figure 4 - Another option is to use a small step as shown aboveand slowly lower the inside of your foot off the step and then slowly raise it back up so the sole of the foot will be facing in towards the opposite leg.
A
ll in all, an injury that you definitely want to address early rather than push through
Please let me know your experiences with ‘shin splints’ and what worked for you!
Jimmy:
ReplyDeleteYou invited readers to "Please let me know your experiences with ‘shin splints’ and what worked for you!" Unfortunately, I'm not sure if this means "Post a comment." I tried various other options on the site, but none of them seemed appropriate. (What does "Join this site" mean? My Google email password certainly didn't work, although the site displayed my email address) Perhaps a simple "Contact me" button is required? As a reader, I don't necessarily want my communication with you - which might expose my ignorance or stupidity - to be available to just anyone. Of course, I don't necessarily expect a personal reply, either. Maybe the site should specify whether the comment gets moderated by you before it gets posted on the site?
All this being said, I'd like to thank you for the insight you have provided on shin splints. Unfortunately I can't tell you "what worked for me." I've only done an initial reading of your article, but it certainly looks useful. While digesting it more thoroughly, I thought you or readers might be interested in my musings to date on the condition. I'm now 65, and have been running for more decades than I care to remember, but I've only experienced shin splints in the last 12 months or so. My running mate insists it's all a matter of shoes. I've run in a wide variety of shoes over the decades - and still do - but have never had the problem until now. That suggests to me that age is a far more likely factor - although that doesn't help a lot: it suggests that stopping running may be the only solution. The fact that the condition comes and goes quite capriciously, apparently independent of training loads, training intensity or training down-time, suggests that other lines of enquiry may prove more fruitful. Before I read your article, I wondered for example if other variables in my training could constitute precipitating factors, such as weather (below-freezing?), injury (muscle? bone?), terrain (soft? hard?) "shin-splint anxiety" (whether - or when - the condition will strike), or cross-training (when I transition from a run to walk during the same training session, the condition persists for some time).
I'll let you know how I progress.
Best wishes
Sean
Hi Sean, I completely understand the contact information issue. It's something most of us have to consider these days. This site is evolving and I'll do my best to make it as user friendly as i can. I do appreciate the feedback.
DeleteWith regards to your tibial pain "shin splints", this type of injury usually follows a fairly predictable pattern. That is, it warms up after a a period of discomfort in the first part of the run, only to get worse towards the end or cessation of running. It usually hangs around after the training session and as it progresses will be sore the next day. If training is continued then it will not warm up and continue to be painful through out the run.
Your pattern of pain does not seem to be predictable - there may be other factors at play. You might consider nerve related pain in particular the deep tibial nerve as this nerve travels deep in the calf having it's interface (adjacent to) the tibialis posterior.
This particular muscle is a factor involved as a causative factor in tibial pain especially when you consider it is a stabiliser of foot mechanics and the lower limb. I do wonder what is happening at your hip and therefore your lower lomb mechanics as you run?? I doubt it is simply a matter of shoes.
With regards to the aging factor, yes things do slowly degenerate over time and we cannot ignore the aging factor however you would have to ask yourself 'why now' after all the years of running has this occurred? Has there been a change in biomechanics? Have you had a previous 'niggle' that has changed your running style (even just slightly). Does this occur when you run faster - this usually changes mechanics, if it does change - this might be part of the problem.
From a clinical stand point i have seen results with people going to softer surfaces even though science might tell us otherwise. Some studies suggest similar peak forces on soft surfaces to hard surfaces (it just takes longer to get there). If you are running in below freezing temps - that's cold! The same pattern will occur it just might take a few more minutes to warm up.
Another factor to consider is the longer this goes on the longer it takes to respond to treatment. This type of injury can be a long term problem as you are no doubt finding out. Soft tissue and or boney changes may start to occur in prolonged cases and this is where imaging can certainly help. In your case and in most cases the cause is likely multi factorial where a number of things will contribute.
Take the time to address
Foot mechanics - professional advice
Hip stability while you run - do you know someone who can watch/video this?
Muscle imbalances - what else is occurring through the chain when you run
Shoes??
Do you get regular soft tissue treatment?
Are you tender in the middle to lower one third of tibia on palpation - compare one side to the other - this may give you an indication of medial tibial pain
I hope this helps!
I you would like further information please contact me by email
jimmybarker9@gmail.com
Great article and would love your comments on our blog. What are your thoughts on compression as part of the RICE treatment method, specifically when applied to shin splints treatment?
ReplyDeletehttp://blog.bodyhelix.com/2012/02/shin-splints-mtss-and-cecs.html
I anticipate that taping would assist one with proprioception and hence aide the sufferer in that respect but compression is a whole new approach.
Clinton
www.bodyhelix.com.au
Hi Jimmy, great article
ReplyDeleteAy experiences are: Last year I started playing AFL football after a few years break. After 2 training sessions I had shin pain. I took time off, returned to training and still had pain. I battled through it for 5 months. When the season ended I went to see a physio who performed massage and acupuncture. It didn't seem to help and was expensive so I stopped. I had 5 months of relative rest. The rest didn't seem to help, even when walking on an incline the pain was there.
The AFL season is starting up again now. My shin pain is still there but I have come up with a technique to deal with it. Before the start of training I take 2 asprin, during training I wear compression socks, after training I apply ice. I have been doing this for 2 months: at the start I only did 1 training session a week but I have gradualy increased and am now doing 2 per week. Games are just starting now and I am planning to do 1 training & 1 game per week to start building to 2 training + game later in the season.
Although my technique allows me to get through training, the pain experienced the next couple days is quite bad. My question is whether this approach is sustainable and what are the longterm factors (will the shin bone get stronger or am I risking serious injury)?